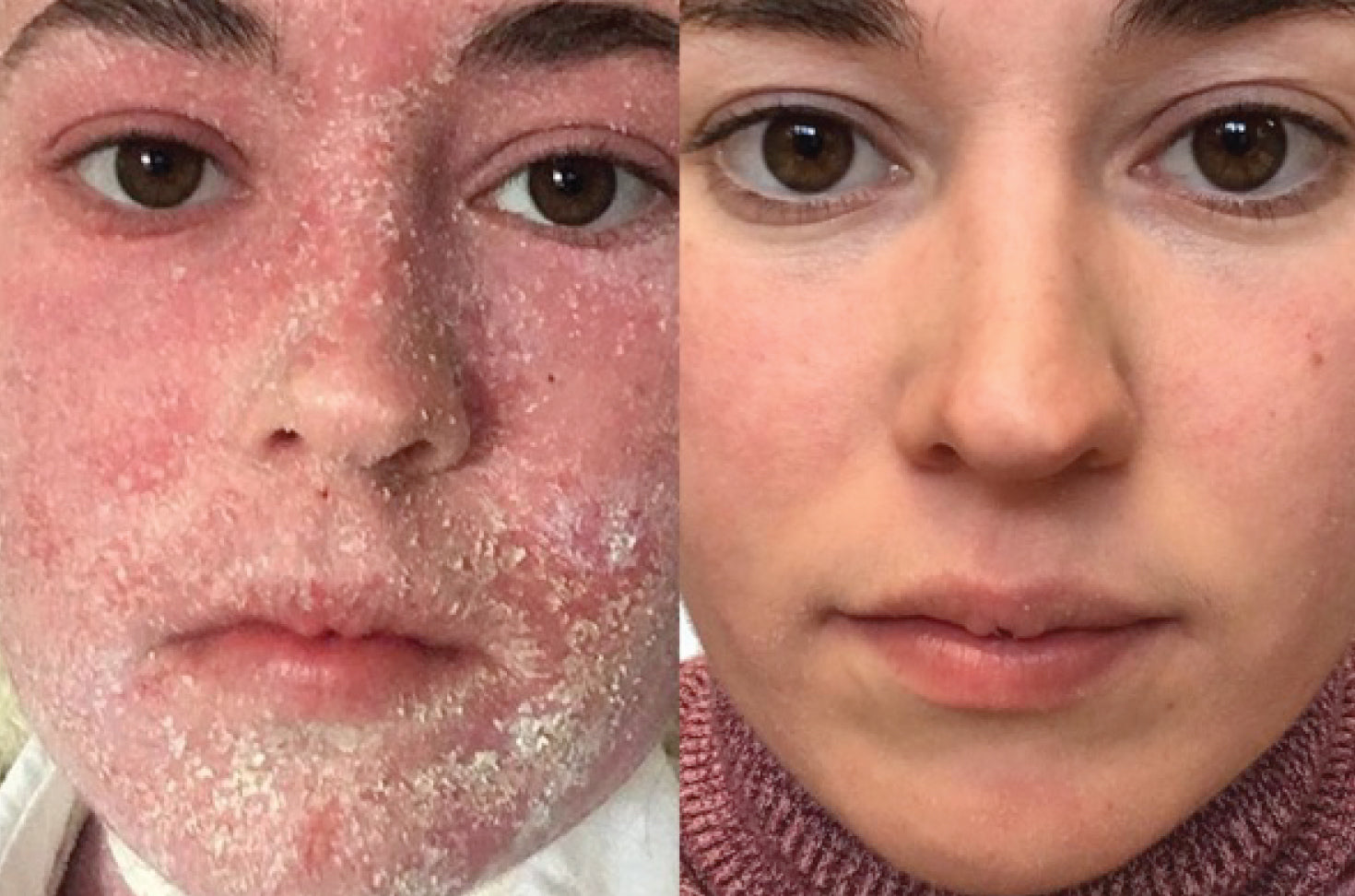
Topical steroid withdrawal is a horrific thing to go through; even those lucky enough to get to clear skin within months rather than years suffer hugely during the process. Everything hurts, everything is painful, everything is challenging, including people’s mental health and self-confidence. TSW means living with sore, flaking, oozing skin, being in constant discomfort, missing friends, losing work, not being able to go out or enjoy a normal life… nothing about it is an easy choice.
So the language that is used to talk about the condition really matters.
How does it get characterised? As ‘steroid misuse’. Or ‘steroid abuse’. We sometimes refer to as ‘topical steroid addiction’, which, even it’s if not meant to imply that people going through TSW are addicts, generally doesn’t really make clear that the issue is with the body’s immune system response being damaged by the steroidal suppression of inflammation, rather than the moral fibre of the sufferer.
People going through topical steroid withdrawal aren’t ‘abusing’ either drugs or their bodies. They’re not sportsmen taking steroids illegally to boost performance.They haven’t done this to themselves. The steroids they used on their eczema weren't ‘overused’, ‘misused’, or used ‘inappropriately’, all of which terms are regularly seen in news reports or articles about the condition. They were used as directed by a doctor.
People going through TSW not at fault, and the language we use to discuss the condition really needs to reflect this.
The fact is that these are people who have been prescribed the standard treatment for eczema or other chronic skin conditions. They’ve been prescribed steroid creams by medical professionals who themselves have generally followed official advice regarding what potency and what time scale they should be used. To suggest that anyone who’s suffering from steroid-induced red skin syndrome (RSS) has not followed their doctor’s advice, has made a mistake, has applied steroids in an inappropriate or wilfully careless way, is horribly insulting.
You could even say that it’s victim-blaming.
So here’s our position on the subject: topical steroid-induced dermatitis is not a choice. It is not a mistake on the part of the patient. And while it is, thankfully, relatively rare among eczema sufferers, it is not half as rare as was once believed. And certainly it’s not so rare that guidelines around the routine prescription of steroids should not be changed to take account of the devastating consequences of steroidal damage.
We would also question the use of 'red skin syndrome' or RSS to describe the reaction when topical steroids are stopped; it is problematic and excluding to use a term that refers to the colour of inflammation on white skin, when the same condition does not show up as red on people of colour. We think that the term 'topical steroid withdrawal syndrome' (as preferred by ITSAN) describes the condition best, but the medical profession also refers to 'steroid-induced dermatitis', 'steroid-induced erythema' or 'steroid-induced rosacea' to describe the same set of symptoms.
Thank you to @tsw_hollybee for the photo used on this page. Follow Holly's TSW journey on her instagram page.