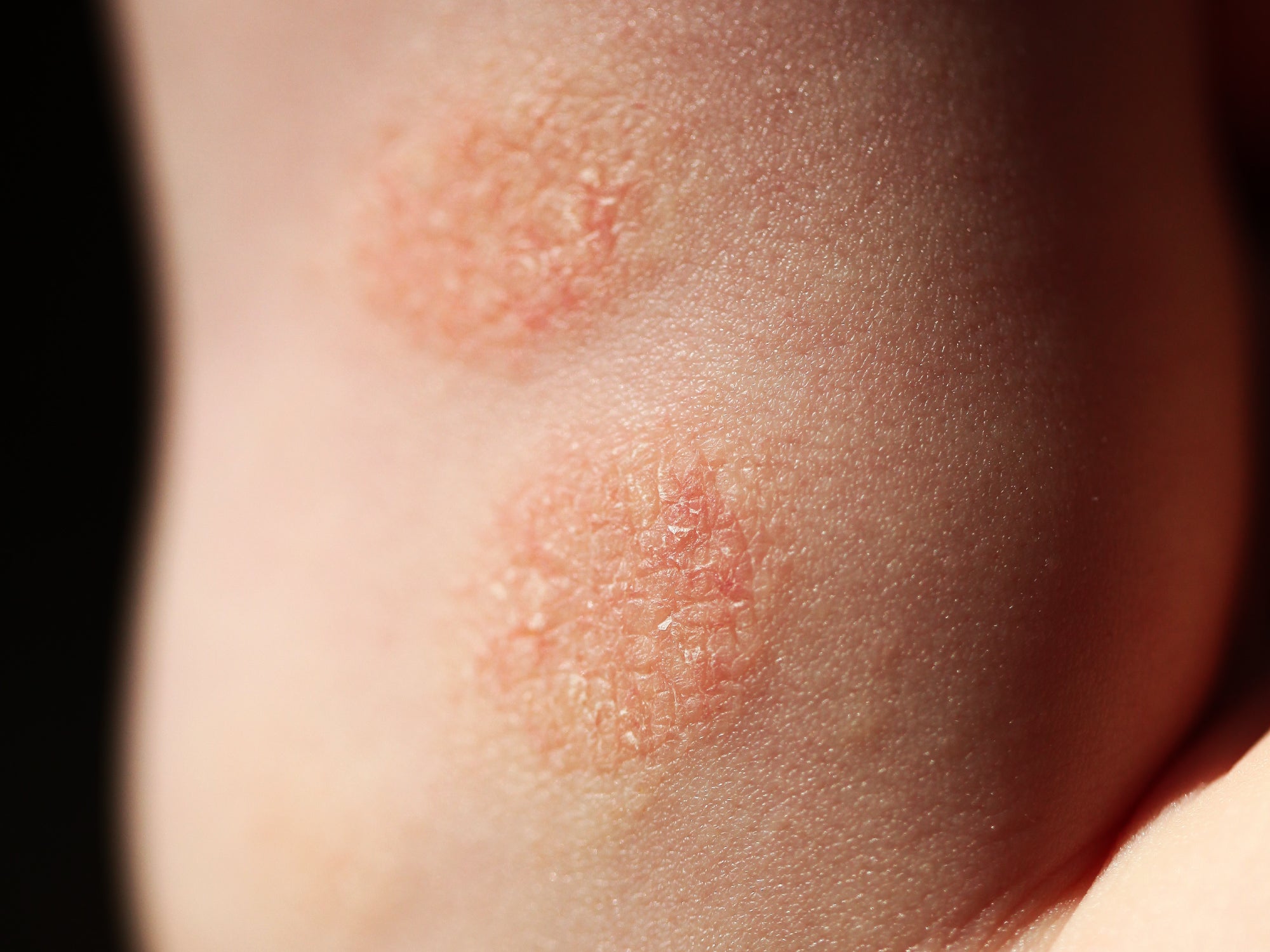
What is discoid eczema?
Discoid eczema is one of many variants of atopic dermatitis (ie eczema), primarily characterised by its distinctive appearance. As its name suggests, discoid eczema appears in disc-shaped patches; it’s also known as ‘nummular eczema’ for the same reason, ‘nummular’ meaning coin-shaped.
These patches of eczema can be round or oval, and like other types of eczema, tend to feel itchy, dry and sore. Discoid eczema can affect anywhere on the body, although it rarely appears on the face or scalp. Because discoid eczema is a chronic condition, patches are likely to come and go, with the eczema reappearing on the same part of the body each time. Treatment is focused on managing the condition rather than curing it.
What are the symptoms of discoid eczema?
This type of eczema tends to start as small spots, blisters or bumps on the skin; these bumps then expand outwards into circular patches of dry, inflamed skin. Often, the centre of a patch can clear up as the affected area expands, and it’s the outer edge that are most inflamed, itchy and sore. The intense itching often gets worse at night. Affected patches tend to be differently coloured compared to surrounding skin: darker brown, purple, grey, pink or red depending on your usual skin tone.
Although discoid eczema looks quite distinctive, it can sometimes be confused with other circular patterned skin conditions, particularly ringworm (which is in fact a fungal infection), so do get a diagnosis from a medical professional before treating it.
What causes discoid eczema?
Like other types of eczema, the root cause of discoid eczema is unknown; it’s unclear why some people are susceptible to developing it, while others are not.
However, there are some specific factors which seem to trigger a flare of discoid eczema:
- Dry skin/impaired skin barrier function
- Irritant ingredients in toiletries
- Insect bites
- Injury to the skin
- Burns
- Some medications (particularly some used to treat arthritis, high cholesterol and Hepatitis C)
- Dry environments
- Cold environments
- Stress
- Middle-age
- Poor circulation
Preventing discoid eczema
It can be very difficult to prevent discoid eczema if you’re someone prone to developing it, as some of the factors we’ve mentioned are going to be totally out of your control! However, it’s possible to be aware of what your triggers are and work towards reducing the risk for yourself.
That might mean taking extra care to protect yourself from insect bites if you’re going somewhere hot or humid, checking with your doctor before being prescribed medication, and being aware of how the temperature and humidity of your living environment affects your skin. You might have to find some effective stress management techniques to lower the inflammatory effect of all those stress hormones on your skin, or talk to your doctor about improving the circulation in your lower legs.
It will also mean being really conscious of what’s in your toiletries and household cleaners! It’s the irritant ingredients in things like shower gels, cosmetics, bubble baths, washing powder, shampoo and hand wash, and surface cleaners that can cause problems to already sensitive skin, so make it your business to check out ingredients, and stick to short and simple lists.
And lastly, because we know that discoid eczema is a problem for people with dry skin, preventing an eczema flare also meant keeping hydrated. Using an intensive emollient every day to keep your skin moisturised is a really useful long-term strategy for reducing the risk of developing discoid eczema.
Managing a flare-up of discoid eczema at home
We’d recommend looking after your skin with natural emollients, keeping it moisturised, nourished and resilient so that any trigger is less likely to set off a flare of discoid eczema. If it’s really itchy, sore or cracked, try Skin Salvation balm, which is less likely to sting on open skin, and can help support the regeneration of a healthy skin barrier. For daily maintenance, use our shea butter and hemp Daily Moisturising Cream, and try countering the dehydrating effects of bathing with some Bath & Body Oil.
If symptoms don’t improve after a week, or get worse, consult your doctor; there are various other options you can try: antihistamines to help ease the itchiness, antibiotics (if the eczema is infected) or a short course of topical steroids if the inflammation is not calming down.
Recommended products:
Balmonds Skin Salvation
with hemp and beeswax
Bath & Body Oil
with lavender, hemp and olive
Balmonds Daily Moisturising Cream
with shea butter and calendula